|
To coincide with Mental Health Awareness Month this May, LIBR would like to share a few key highlights from a lecture on the the State of Mental Health in 2024 presented by Dr. Martin Paulus, Scientific Director and President to LIBR scientific staff earlier in the year.
Q: What are the main challenges in global mental health systems, and what changes are urgently needed? A: Global mental health systems face significant challenges, including being under-resourced and often failing to provide adequate, quality care. There is an urgent need for systemic change, which involves shifting towards community-based care, strengthening health systems, securing political commitment, increasing financing, and leveraging digital technologies to enhance mental health services. Q: How prevalent are mental health issues in the U.S., and what are the barriers to accessing care? A: Mental health issues are widespread in the U.S., with over 50 million adults experiencing them, akin to the combined populations of New York and Florida. Despite this, more than half of these individuals do not receive treatment due to high costs and lack of insurance. Nearly 30% of adults with mental illness cannot seek treatment due to affordability issues, highlighting a critical gap in mental health care. Q: Why is a personalized approach crucial in treating depression? A: Depression manifests in varied forms and severities, influenced by a mix of individual risk and resilience factors. A personalized approach is crucial as it ensures that treatment is tailored to each person’s unique experiences, preferences, and life context, leading to more effective recovery. Involving individuals with lived experience in care decisions also enhances accountability and the efficacy of healthcare systems. Q: At what ages do psychiatric disorders typically onset, and what are the implications for mental health services? A: Psychiatric disorders often onset early, with one-third starting before age 14 and about half by age 18. This underscores the importance of early intervention and integrating mental health promotion and prevention into schools, colleges, and healthcare settings. Mental health services should support integrated care models for transitional age groups, ensuring continuous care without age thresholds. Q: How do risk and protective factors influence depression, and what strategies can be used for prevention? A: Risk factors for depression include significant life changes such as widowhood, childhood abuse, and poor physical health, while protective factors include a healthy diet rich in zinc, tea, and fruits. Strategies for prevention should address these varied factors comprehensively, helping healthcare professionals identify high-risk individuals and customize interventions to prevent or mitigate depression. Q: How do work-from-home trends and social isolation impact mental health? A: Work-from-home trends have increased, with 34% of people working from home in 2022. While this can offer flexibility, it may also contribute to social isolation and loneliness, which are linked to higher risks of premature death, heart disease, stroke, anxiety, depression, and dementia. Reducing social isolation by fostering community involvement and social connections is crucial for improving mental health. Q: What integrated solutions are recommended to address mental health challenges effectively? A: Integrated solutions include implementing early screening programs, promoting healthier living and working environments, increasing investment in mental health resources, and fostering social connections. Additionally, employing evidence-based methodologies to monitor treatment outcomes and conducting public awareness campaigns to change perceptions around mental health can significantly improve mental health care and support.
0 Comments
In 2023, LIBR investigators published over 120 peer-reviewed research articles. In conjunction with the release of our annual report, we asked each principal investigator to weigh-in on their lab's highlights over the past year. Here's a snapshot of some of the outstanding accomplishments:
Robin Aupperle The NeuroCATT lab received an R34 award from the National Institute on Alcohol Abuse and Alcoholism (NIAAA) in collaboration with Dr. Charles Taylor at the University of California San Diego and Dr. Kate Wolitzky-Taylor at the University of California Los Angeles. The grant will fund work furthering the development of an intervention focused on amplification of the positive valence system and reducing alcohol use (AMP-A) for individuals with alcohol use disorder and symptoms of anxiety or depression. The first phase of the project involved collecting input from substance use providers and prior participants concerning the intervention and piloting the treatment with eight individuals. This will lead into a randomized clinical trial comparing the novel intervention with a more traditional cognitive-behavioral therapy intervention. Chun-Chieh Fan Dr. Fan was invited to moderate a panel on the genomic analysis of the human brain data at the American Society of Human Genetics held in Washington, D.C, published a special issue on genetic data from the Adolescent Brain Cognitive Development Study in Behavior Genetics and was invited to give a workshop on geospatial dat analysis at the BERTHA summer school in Denmark. Salvador Guinjoan Dr. Guinjoan’s lab completed the recruitment of 20 persons who suffer from major depression and varying degrees of rumination intensity, and expect to complete recruitment of 10 persons who are healthy and will serve as a comparison group for the low-intensity focused ultrasound (LIFU) pilot study targeting white matter tracts in the anterior limb of the internal capsule in the right brain hemisphere. The lab observed consistent target engagement with this method in a preliminary analysis, and a trend towards resulting clinical effects. This was the first time that white matter tract functional modulation had been demonstrated with a noninvasive method such as LIFU, which before was only possible with costly, invasive, and risky methods involving electrode implantation or tissue ablation. This observation will allow for the testing of additional participants with the goal to make causal inferences about brain mechanisms of symptom generation in major depression and other psychiatric disorders. Maria Ironside Dr. Ironside was awarded a $2.1 million 5-year R01 grant from the National Institute of Mental Health to investigate “Processes and circuitry underlying threat sensitivity as a treatment target for comorbid anxiety and depression.” The study employs a pharmaco-fMRI approach to study threat sensitivity using a novel predator task in patients with major depressive disorder (MDD), anxiety disorders (AD), and comorbid MDD and AD. The ultimate aim of this work is to establish treatment targets for comorbid MDD and AD for novel interventions and provide evidence for the separation of MDD from comorbid MDD and AD in future clinical trials. Sahib Khalsa An ingestible vibrating capsule produced reliable changes in gastric-evoked brain activity and stomach sensation in healthy individuals. This minimally invasive mechanosensory approach serves as the basis for an ongoing NIH-funded study focused on identifying abnormal gut-brain interactions in women with anorexia nervosa as well as in individuals with functional gastrointestinal disorders. Martin Paulus Many computational measures have poor psychometric properties, which could invalidate previous findings and hinder ongoing research. The Paulus lab recommended steps to address these issues and facilitate the translation of computational assays to clinical practice. As well, Individuals with MDD have lower expression of miR-93, which is associated with higher levels of certain inflammatory markers. Unlike healthy individuals, those with MDD don’t show an adaptive epigenetic regulation of a brain region (insula) involved in processing internal body signals, hinting at the molecular mechanisms that might be altering brain responsivity to these signals in MDD. Jonathan Savitz Dr. Savitz continued his work with cytomegalovirus (CMV). Drs. Haixia Zheng and Savitz published a paper in Molecular Psychiatry showing that CMV infection is associated with suicide, increased expression of inflammatory markers and microglial “activation” postmortem. As well, the Savitz lab published a Hot Topics paper on herpesviruses and psychiatric disorders in Neuropsychopharmacology. Ryan Smith Dr. Smith began data collection on a new pilot study examining computational mechanisms of breathing perception in anxiety disorders. His lab also continued to make progress on a 3-year project funded by a grant from the Well-being for Planet Earth Foundation. This project investigates neurocomputational predictors of subjective well-being. Data collection was also completed for a study examining the influence of an interoception-based anxiety induction on decision-making mechanisms associated with information-seeking and planning. Jennifer Stewart Compared to individuals with a history of major depressive disorder (MDD) and healthy controls, individuals with amphetamine use disorder 1) report greater positive and negative urgency (taking rash action when feeling good or bad); and 2) exhibit greater right hemisphere brain signals (in right anterior/middle insula, amygdala, and ventral striatum) during successful behavioral inhibition. These findings point to heightened impulsivity during emotional arousal and recruitment of more brain resources to exert inhibitory control. Wes Thompson Dr. Thompson gave a talk at the Joint Statistical Meetings on August 7, 2023, on “Annotation-Informed Polyvertex Scores for Brain-Wide Association Studies", served as the managing guest editor for a special issue of Developmental Cognitive Neuroscience on novel methods for population neuroscience, and continued his efforts as Director of Biostatistics for three national consortia on longitudinal neurodevelopment: the National Consortium of Alcohol and Neurodevelopment in Adolescence (NCANDA), the Adolescent Brain Cognitive Development (ABCD) Study℠, and the HEALthy Brain Child Development (HBCD) Study. Evan White LIBR received a DP1 grant for research to be conducted by Dr. White in collaboration with the Shawnee Tribe of Oklahoma titled “Kipiyecipakiciipe – Coming Home: Establishing clinical cultural neuroscience as a tool for understanding the role of traditional cultural engagement in mitigating substance misuse and disorder.” Within American Indian (AI) populations, there is a disproportionate share of negative health and social consequences of substance use disorder (SUD) even after decades of awareness and research. This project aims to integrate community-based participatory research (CBPR) with neuroscience tools to examine the influence of traditional cultural engagement on resilience factors that may protect against poor mental health as well as risk for substance use. Dr. Sahib Khalsa, M.D., Ph.D., is Director of Clinical Operations for LIBR, Associate Professor at the Oxley College of Health Sciences at the University of Tulsa, Director at LIBR Float Clinic and Research Center, and Volunteer Faculty Member in the Department of Psychiatry at the University of Oklahoma. Dr. Khalsa’s laboratory studies the role of the brain-body connection in human health; he has published more than 90 peer-reviewed papers and has received research funding from the National Institute of Mental Health (NIMH), National Institute for General Medical Sciences (NIGMS), National Center for Complementary and Integrative Health (NCCIH), the NIH/National Center for Advancing Translational Science (NCATS), the Mind and Life Foundation, and the Brain and Behavior Research Foundation. His research is currently funded by NIMH and LIBR.
Q: The Laureate Psychiatric Hospital and LIBR are known and respected for their work in the fields of identifying, treating, and researching eating disorders like anorexia nervosa; as February is focused on heart health, how does what you study relate to a healthy heart? A: Many people know about the relaxing experience of floating in water or the value of taking some time each day to pause and be away from the usual hustle and bustle of daily activities. We are currently studying the potential therapeutic impact of a particular form of Reduced Environmental Stimulation Therapy (REST) called Floatation-REST, on mental health in individuals with anxiety disorders, depression, eating disorders, or substance use disorder. Floatation-REST reduces external sensory input to the central nervous system by minimizing environmental stimulation, through the act of floating supine in a pool of water saturated with Epsom salt. In this environment, the density of the salt water allows for effortless floating. The temperature of the air and water is matched to the person’s skin temperature, and visual and auditory stimulation and movement is minimized. Our research using Floatation-REST (Paper 1) (Paper 2) has shown that it can significantly reduce blood pressure during the float session, especially the diastolic blood pressure, reduce breathing rate, and certain metrics of heart rate variability, suggesting a shift in the autonomic nervous system toward a more relaxed state. Interestingly, Floatation-REST is also associated with enhanced awareness for cardiac and respiratory sensations while reducing anxiety levels in anxious individuals, indicating a paradoxical effect. We have also recently found that Floatation-REST acutely lowers anxiety and stress symptoms and improves some aspects of body image in hospitalized individuals with anorexia nervosa. Q: How do your present studies take the next steps in studying heart health as it relates to eating disorders? A: Our ongoing studies are adding to the rigor of prior research by thoroughly characterizing the cardiovascular changes induced by Floatation-REST and examining how neural and physiological changes are associated with its anxiolytic effects. For example, in healthy individuals, we have found that Floatation-REST is associated with a reduced functional coupling of brain activity within the hubs of brain networks most responsible for creating and mapping our sense of self. We also recently found that women with anorexia nervosa show reduced brain-body network connectivity after undergoing a cardiac stress challenge; the less connected these parts of the brain were, the more anxiety, depression, and negative body image the women had. We plan to extend these studies to identify whether changes in similar brain networks helps to explain the beneficial impacts observed with Floatation-REST in individuals with eating disorders. Q: Do you need people to help you with this research project? A: We are conducting several studies looking at the role of the brain-body connection in eating disorders. When an individual receiving treatment with Laureate qualifies for ongoing research studies, they may be offered the opportunity to participate. The clinical team assists in evaluating how participation will support their recovery and whether the individual might benefit from engaging in the study. We also need volunteers not in treatment for an eating disorder to help with this research. If you or someone you know between the ages of 13-40 would like to be one of our paid volunteers, please contact our lab or fill out the form on our website. Now that the initial fervor of New Year’s Resolutions has passed, you have plenty of time to consider what is most meaningful to you and develop goals that may truly fit with those values.
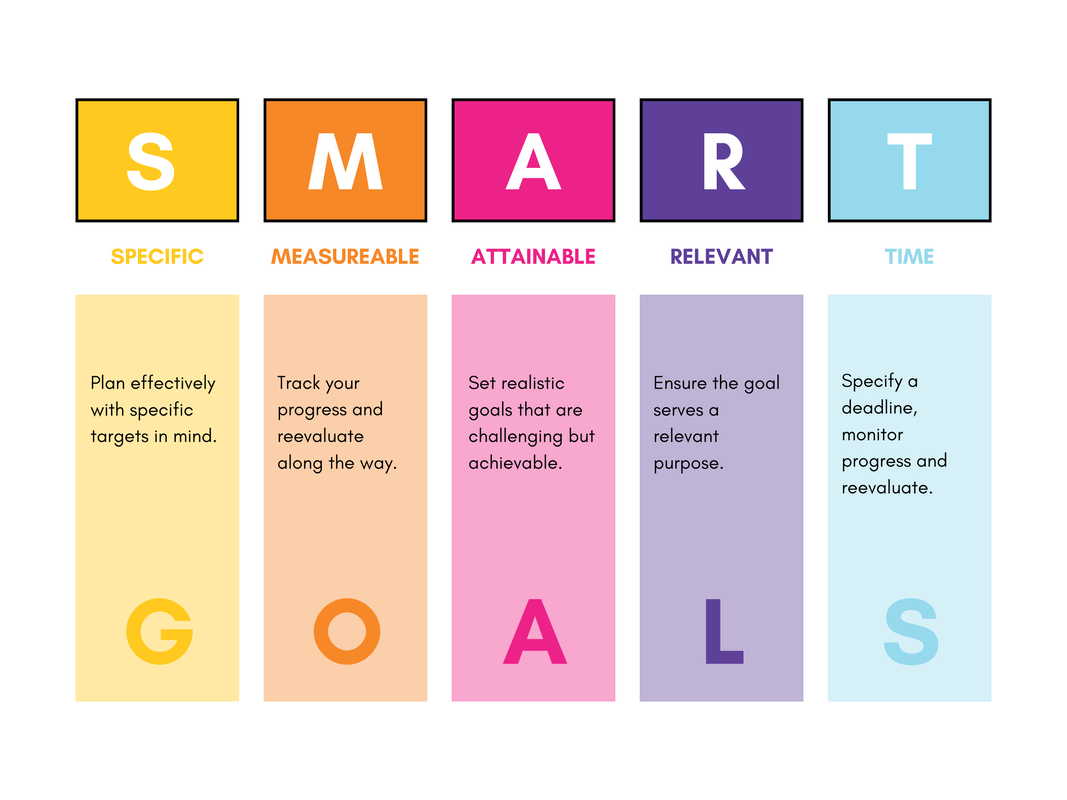
We talked with LIBR principal investigator Dr. Robin Aupperle about how to combat the tendency of people to abandon their January 1 resolutions—and instead use SMART goals to make lasting life changes. Q: How are SMART goals different from something like a New Year’s resolution? RA: Good question. There’s a tremendous push—internal and external—to start the New Year with a big, transformative resolution. For instance, I’ve heard resolutions like “I’m going to work out every single day this year,” “I’m going to save 50% of my salary,” or “I’m going to lose 50 pounds,” none of which are likely to be realistic. Some of these goals may also relate to what people feel they “should” do rather than necessarily being related to what is truly important for that individual. Q: Those seem lofty, but if we don’t try, we’ll never do it, right? RA: It can be very challenging to change our behaviors and ingrained habits. In order to be successful, the new behaviors have to be rewarding and reinforcing in some way. This feeling of reward can come from feeling successful and accomplished for being successful, or from engaging in something we value and enjoy. Q: What’s a better approach? RA: SMART goals offer a great framework for how to think about goal-setting. SMART is an acronym that helps identify and quantify elements of the goal you’re setting. Q: How does that work? RA: SMART stands for: S Specific What is the specific goal that someone wants to accomplish? “I want to increase my stamina and endurance so that I feel healthier.” M Measurable What data will be used to measure the goal? How will I measure it? “I will start by doing something that raises my heart rate for 20 minutes two times a week. My long-term goal will be to work towards 30 minutes, three times per week. I’ll make a calendar to chart my progress and keep myself accountable.” A Achievable Is the goal doable? Do you have the necessary skills and resources? “I will walk around my neighborhood (around the office, or at the mall) after work on Mondays and Thursdays, inviting friends to join me.” R Relevant How does this goal align with your values? Why is the result important? “I know I need to be less sedentary for my health. I want to be healthier in order to feel like I have more energy throughout my daily life and live longer.” T Time-Bound What’s the timeframe for accomplishing this goal, beginning to end? “I will focus on 20 minutes, two times a week for two months and assess my progress and modify my goals as needed.” Q: That’s a lot of work! RA: Much of this relates to all the thoughts going on in our heads when we are considering behavior change. This just provides a framework for organizing these thoughts, and making them specific. The main idea though, is that any attempts at change offer helpful information. If you aren’t successful in your first attempts, the key is to not get down on yourself! Simply consider what obstacles got in the way and how you can modify your plan to be more effective. For example, this could include starting smaller and breaking things down – for example, starting with walking around the block ONE time, ONCE per week to begin with….and then working up from there. Any amount of successful change goes a long way towards motivating further change. The University of California created this SMART goals template—it’s really good. You can use it to write your own SMART goals: Initial Goal (Write the goal you have in mind): ______________________________________________________________________________ 1. Specific (What do you want to accomplish? Who needs to be included? When do you want to do this? Why is this a goal?) ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ 2. Measurable (How can you measure progress and know if you’ve successfully met your goal?): ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ 3. Achievable (Do you have the skills required to achieve the goal? If not, can you obtain them? What is the motivation for this goal? Is the amount of effort required on par with what the goal will achieve?): ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ 4. Relevant (Why am I setting this goal now? Is it aligned with overall values?): ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ 5. Time-bound (What’s the deadline and is it realistic?): ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ S.M.A.R.T. Goal (Review what you have written, and craft a new goal statement based on what the answers to the questions above have revealed): ______________________________________________________________________________ ______________________________________________________________________________ ______________________________________________________________________________ Q: Do you have any SMART goals you’re working on? RA: I am working towards building strength by focusing on lifting weights when I am at the gym. My initial goal is to go twice per week for 30 minutes each time. I am going to re-assess my goals in two months to consider if I should modify my goal. This is important to me because I want to be stronger to keep up with my kids, who are very into ninja warrior right now! I also have non-health related goals, such as writing a children’s book, which I have broken down into several steps needed to work towards that goal. Dr. Aupperle has initiated research projects at LIBR investigating neurocognitive and behavioral predictors of treatment response to behavioral activation therapy for depression and exposure therapy for anxiety. In addition, she is taking the lead in LIBR projects investigating predictors of success for females enrolled in a criminal diversion program and factors related to mental health resiliency in college students. What are the most common ways the holidays can trigger stress, anxiety, and sadness?
What can I do to minimize stress? The key word is ROUTINE, the other, CHOICES.
Q: What is this research about, and what are you hoping to learn?
A: We are doing a study to see if a special supplement, kind of like the keto diet, can change how the brain works in people with depression when performing tasks about good, bad, and personal experiences. It will take about 10-11 weeks to get all the information we need for this study. Q: Who is the ideal candidate to participate in this study? A: To be in this study, you should be feeling depressed. If you take medicine, you need to have taken the same amount for at least 6 weeks before joining the study. But don't join if you're pregnant, might be pregnant, or want to get pregnant soon. Also, if you're breastfeeding, want to take vitamins or change your diet during the study, have heart or kidney problems, another ongoing health issue, feel like hurting yourself, or are very scared of tight spaces, it's best not to be in the study. Q: What happens to people who take part in this research? A: We need up to 75 people for our study. Everyone will have a talk with a mental health expert, answer some questions, do brain games, get pictures of their brain, give blood and urine samples, and try either a special diet-like drink or a placebo for two months. Q: How do you decide who gets the keto-like supplement, and who gets the placebo? A: In this study, whether you will get the supplement or a powder that does do not anything is like flipping a coin. Half of the people will get the special drink, and the other half will get a pretend one. You and the doctor won't know which is which, but they can find out in case of an emergency. Q: Could being involved in this research hurt me? A: No, this study is low risk, but there are a few things that might not feel so great. First, the special drink could give you an upset stomach, nausea or diarrhea. Second, when they take your blood, it could pinch a little. Lastly, when you go into the machine for pictures, you might feel a bit claustrophobic or nervous. But don't worry, if anything bothers you, just tell the people doing the study, and they may be able to help you feel better. Q: I’ve never had an MRI. What’s that like? A: The brain pictures are taken with a special machine called an MRI. An MRI does not involve any radiation, unlike an X-ray. The MRI machine looks like a big metal tube with a strong magnetic field around it. You'll lie on a table that goes into the tube. It's important to stay as still as you can while the machine takes pictures. It can be noisy, so you'll have earplugs to make it quieter. You can talk to the people running the MRI, and if you want to stop, they'll help you get out. They may also keep an eye on your heart rate and how you breathe using a small device on your finger and a band on your chest, but it won't be tight. Q: Will being involved in this research benefit me? A: You might not see direct benefits for yourself in this study, but you're doing something really important. By being part of this research, you're helping us learn more about a keto-like supplement and how it affects the brains of people with depression. This information could be used to help others with depression in the future, so your participation is valuable for everyone. Q: How long will each study visit take? A: Each study visit may vary in length, but on average, it will take a few hours. We'll do our best to schedule appointments that work for you. Q: Will I need to come to the study site for every visit? A: Yes, you'll need to come to the study site for most visits. We want to make sure we can closely monitor your progress and collect the necessary data. Q: Are there any dietary restrictions during the study? A: While you're in the study, it's important to follow the instructions provided regarding your diet. You may be asked to avoid certain foods or beverages. Q: Will I receive any compensation for participating in the study? A: Yes, we'll provide compensation for your time and participation in the study. The amount will be discussed with you during the informed consent process. Q: What if I have to miss a study visit? A: If you need to miss a study visit, please let the study team know as soon as possible. We'll work with you to reschedule and make sure you stay safe and healthy during the study. Q: Will my personal information be kept confidential? A: Yes, your personal information and data will be kept confidential. We take your privacy seriously and will follow strict guidelines to protect your information. Q: How will I receive updates on the study's progress? A: You can ask the study team for updates on the study's progress, and we'll do our best to keep you informed throughout the research. Q: I’d like to talk to someone about participating in the study. What should I do? A: Excellent! Please visit our website: ONGOING STUDIES - Laureate Institute for Brain Research, or call 918.502.5100.  As a postdoctoral research scholar at LIBR, Dr. Hannah Berg, Ph.D. is dedicated to investigating the brain basis of decision-making in clinical anxiety. The long-term goal of this work is to provide insights that will help clinicians deliver more effective interventions. Dr. Berg’s clinical training in the treatment of obsessive-compulsive disorder (OCD) has inspired her to develop a program of research focused on OCD and its characteristic behavior patterns. What is OCD?
OCD is a mental health disorder that affects people of all ages and walks of life, and involves a cycle of obsessions and compulsions. Obsessions are unwanted, intrusive thoughts, images, or urges that trigger intensely distressing feelings. Compulsions are behaviors an individual engages in to attempt to get rid of the obsessions and/or decrease distress. More information about OCD, as well as resources for treatment, can be found at iocdf.org. What is your research study about? We are investigating the brain basis of various types of decision-making in individuals with and without OCD. The aim of this study is to better understand how compulsive behaviors arise in some individuals but not others. How is the study being conducted? Participants will undergo an initial evaluation for eligibility. Eligible participants will be asked to complete questionnaires about their emotions and experiences, followed by a series of computer tasks involving decision-making. Brain images will be obtained using functional magnetic resonance imaging (fMRI). Why do you want to conduct this research? Treating OCD has been one of my favorite parts of my job. I am consistently impressed by the bravery and vulnerability that patients show when they enter treatment, and it is immensely rewarding to help someone experience freedom from obsessions and compulsions. However, our gold-standard treatments for OCD, including exposure and response prevention (ExRP) and medications, are only effective for about 50-70% of patients. By shedding light on compulsions, I hope that this research will lead to improved treatments for OCD. In particular, ExRP involves a detailed understanding of what a patient thinks and feels before, during, and after they engage in compulsions. To the extent that this research study can help clinicians understand the brain states and psychological states that lead to compulsions, it will lead to more effective delivery of ExRP. Furthermore, insights from this study may lead to the development of new treatments, including psychotherapies, medicines, and neuromodulatory approaches that offer relief from OCD. Are you looking for participants? We will be recruiting participants beginning in November 2023! This is a pilot study, so we plan to recruit a relatively small number of participants, including individuals with and without OCD. If you are interested in participating, you can contact our assessment team here.
How is my privacy protected? I am sharing personal information about myself. We take confidentiality and privacy very seriously at LIBR, information you provide will be protected as outlined by The Office for Human Research Protections (OHRP) for all of our research studies. OHRP provides leadership in the protection of the rights, welfare, and wellbeing of subjects involved in research conducted or supported by the U.S. Department of Health and Human Services (HHS). OHRP is part of the Office of the Assistant Secretary for Health (OASH) in the Office of the Secretary (OS), U.S. Department of Health and Human Services. See their link: http://www.hhs.gov/ohrp/ What do I need to do to participate in a study? If you are interested in one of our studies or would like more information, please call 918-502-5100. One of our clinicians will arrange an interview with you over the phone to help us to determine of the studies are a good fit for you. If so, an in-person interview will be arranged. Entry criteria will vary from study to study. Where can I learn about studies that are recruiting participants? To learn about studies that are actively recruiting participants, please visit the "Ongoing Studies" section of our website or follow us on Facebook. Is there compensation provided for participating in a study? Yes, you will be paid for your time and effort spent participating in a study. What if I sign up for the study, but decide later that I don’t want to participate? Participation in all of our studies is voluntary and you may choose to stop participating at any time. Why do people participate in mental health research? Many healthy volunteers participate in research to help others and contribute to advancement in science. Participants with an illness or disorder often participate to help others too, but also to possibly receive new treatments or additional information about their mental health. Research studies offer hope for many people and an opportunity for scientists better understand dysfunction in mental health and discover ways to benefit others in the future. What is informed consent? Informed consent is the process of providing potential participants with the key facts about a clinical trial before they decide whether to participate. The process of informed consent (providing additional information) continues throughout the study. To help someone decide whether or not to participate, members of the research team explain the details of the study. The research team provides an informed consent document that includes details about the study, such as its purpose, duration, required procedures, and who to contact for further information. The informed consent document also explains risks and potential benefits. The participant then decides whether to sign the document. Informed consent is not a contract. Volunteers are free to withdraw from the study completely or to refuse particular treatments or tests at any time. Sometimes, however, this will make them ineligible to continue the study. All research at Laureate Institute for Brain Research has been reviewed and approved by an Institutional Review and Ethics Board (IREB). What is magnetic resonance imaging (MRI)? MRI is a non-invasive imaging technology that produces three dimensional detailed anatomical images without the use of radiation. It is safe, painless and uses no radiation. The MRI scanner uses a large magnet to acquire pictures of the brain. There are no known side effects of the MRI scanning used at the Laureate Institute for Brain Research. We do not perform MRIs on women who are or who might be pregnant. Additionally, since magnets are attracted to the iron which can be found in some metal products, you will be asked a list of questions that will help us determine if the MRI is safe for you. Some common MRI exclusions are metal braces, pacemakers and body jewelry that cannot be removed. The staff will go over a full list with you during the informed consent process. Watch this 60-second video to learn what happens in the body during an MRI scan: What happens during an MRI scan?
The MRI scanner is composed of a large bed which slides into the cylinder. As the bed slides in, your head and upper body will be in the center of the cylinder for varying lengths of time. The room is cold, so it is best to dress in warm and comfortable clothing. When the machine is working, it can be very loud and makes different kinds of noises. To increase your comfort, you will be given ear-plugs to reduce noise volume. An MRI technologist will run the MRI scanner and research staff will be present in the room adjacent to the scanner. Depending on the research project, you may be asked to perform various tasks in the scanner while your body remains inside the cylinder. This allows the researchers to view the physiological responses of your brain as it performs various functions (this procedure is termed “functional MRI” or fMRI). Occasionally, some people experience nervousness or claustrophobic feelings due to the scanner's small space. If this or any other discomfort occurs you will be able to let the MRI staff know this and the scan can be stopped. It's summertime in Tulsa, OK and this week our temperatures are projected to hit the triple digits. We asked Dr. Martin Paulus to discuss some of the latest research on the effects of heat on mental health and recommendations for what you can do to stay healthy as temperatures rise.
Dr. Martin Paulus is the Scientific Director and President of Laureate Institute for Brain Research (LIBR) and a Professor at Oxley College of Health Sciences at The University of Tulsa. Q: Can excessive heat really affect mental health? A: Evidence does support that theory. Signs that heat is affecting a person can include changes in mood, feeling more irritable, anxious, or depressed than usual. Heat can also make it harder to concentrate or think clearly; it can also disrupt sleep, which can worsen mental health conditions like anxiety and depression. If someone already has a mental health condition, they might find that their symptoms get worse when it's hot. We recently reviewed three peer-reviewed studies; the studies found that when it gets really hot outside, people tend to have more mental health problems. You can read the full studies here, here and here. Q: What are the signs of how heat may be affecting your mental health? A: There are 3 main ways the heat may show effects on your mental health: Physical symptoms: Heat can also cause physical symptoms that affect your mental health. For example, you might feel more tired than usual, have headaches, or feel dizzy or nauseous. These physical symptoms can make you feel anxious or down. Changes in behavior: You might find yourself acting differently when it's hot. For example, you might be more impulsive, or you might have a hard time controlling your anger. Worsening of existing mental health conditions: If you already have a mental health condition like depression, anxiety, bipolar disorder, or schizophrenia, you might notice that your symptoms get worse when it's hot. Note: Some people take medication to help with their mental health problems. But when it's hot outside, these medications might not work as well, or they might have more side effects. Doctors need to keep this in mind when they're helping patients during hot weather. Q: How intense can these behaviors become? A: Unfortunately, thinking about suicide is something to be aware of. We do still need more research, but these studies found that when the temperature goes up, sadly, so do suicide rates. This seems to be especially true for men and older people. This means that when we're trying to prevent suicide, we should think about how hot weather might be making things worse. Additionally, people who already have mental health problems might feel even worse, and they might need to go to the hospital more often. This means that hospitals and clinics need to be ready for more patients when there's a heatwave. Q: Climate change is making hot days and heatwaves more common. Is there a concern that there’s a relationship between climate change and mental health problems? A: Yes. One of the studies even predicted that if we don't do anything about climate change, there could be thousands more suicides in the US and Mexico by the year 2050. Q: What else do we need to consider? A: Even though these studies tell us a lot, there's still a lot we don't know. We need more research to understand how hot weather affects different types of mental health problems, what the "danger zone" temperature might be for mental health, and how being inside vs. outside might make a difference. Overall, these studies show that hot weather and climate change can make mental health problems worse. This is a big deal, and it's something that doctors, hospitals, and people who make health policies need to pay attention to. We also need more research to help us understand and deal with this problem better. Q: What can people do to help manage their symptoms and stay more comfortable in extreme heat situations? A: Stay hydrated: Dehydration can worsen feelings of anxiety and irritability. Make sure to drink plenty of water throughout the day, especially if you're sweating a lot. Stay cool: Try to spend time in air-conditioned places if possible. If you don't have air conditioning at home, consider visiting a public place that does, like a library or shopping mall. You can also use fans, take cool showers, or use cold packs to help cool down. Avoid the hottest part of the day: If possible, try to stay indoors during the hottest part of the day, usually between 10 a.m. and 4 p.m, but often later in the Tulsa area. If you need to be outside, try to stay in the shade. Wear appropriate clothing: Wear lightweight, loose-fitting clothing to help stay cool. Light-colored clothing can also help reflect the sun's rays. Take care of your physical health: Make sure to eat balanced meals and get plenty of sleep. Both can help manage mental health symptoms. Practice stress management techniques: Techniques such as deep breathing, meditation, and yoga can help manage feelings of stress and anxiety. Reach out to others: If you're feeling down or anxious, don't hesitate to reach out to friends, family, or a mental health professional. They can provide support and help you find ways to manage your symptoms. Follow your treatment plan: If you have a mental health condition and are under the care of a healthcare provider, continue to follow your treatment plan. If your symptoms are getting worse, contact your healthcare provider. They may be able to adjust your treatment plan to help manage your symptoms during periods of extreme heat. Want to know more? Here's a podcast segment on climate change and mental health with Dr. Nick Obradovich on NPR's 1a podcast and a Mashable article focused on similar research. |
Archives
July 2024
Categories
All
|
VISIT LIBR6655 South Yale Ave. Tulsa, OK 74136
918.502.5100 | [email protected] |
|
© 2009-2024. All Rights Reserved. Laureate Institute for Brain Research
Site powered by Laureate Institute for Brain Research


















 RSS Feed
RSS Feed